Are you ready to grow up your business? Contact Us
Call us anytime
Are you ready to grow up your business? Contact Us
When a patient presents with an acute myocardial infarction, your focus is on immediate intervention. But after the procedure, the way CPT code 92941 is documented and billed determines whether you get paid or face a denial.
This code is heavily audited. Even small documentation gaps can lead to downcoding or full denial. The issue is not the procedure. It is how clearly the emergency is proven in the record.
This guide explains CPT code 92941 with precise billing rules, real-world risks, and practical steps to protect your revenue.
CPT code 92941 has strict criteria. It is only valid when the patient is experiencing an acute myocardial infarction and requires immediate intervention.
Payers review these claims closely because reimbursement is higher than standard PCI codes. If the documentation does not clearly prove an acute MI, the claim is often downcoded or denied.
A common real-world issue is wording. Notes may state “urgent PCI,” but do not confirm an acute MI. From a payer perspective, urgency alone is not enough.
Another pattern is misuse in stable cases. Some practices use 92941 for severe blockages without evidence of an acute event. This almost always leads to downcoding.
CPT code 92941 is used for emergency PCI performed during an acute myocardial infarction.
It includes angioplasty, stent placement, and even atherectomy when performed in the same vessel.
A critical rule must be clearly understood. This code applies to one culprit vessel only. Even if multiple lesions are treated within that vessel, it is still reported once.
The defining factor is not complexity. It is the presence of an acute MI and immediate intervention.
The culprit vessel is the artery responsible for the acute myocardial infarction. This is the vessel causing the active ischemic event.
CPT code 92941 is reported only for this single vessel.
If additional vessels are treated during the same session, they are not included under 92941. These may be reported using other PCI codes, depending on payer rules and NCCI edits.
Failure to clearly identify the culprit vessel in the operative note is a major audit risk.
This distinction is more precise than “emergent vs urgent.”
CPT code 92941 is based on the presence of an acute myocardial infarction, not just the timing of the procedure.
A case can be urgent but still not qualify for 92941 if there is no documented acute MI. In those cases, standard PCI codes such as 92928 should be used.
For example, a patient with severe coronary blockage who undergoes PCI later the same day without evidence of an acute MI does not qualify for 92941.
The safest rule is simple. If there is no clear documentation of acute MI, do not use 92941.
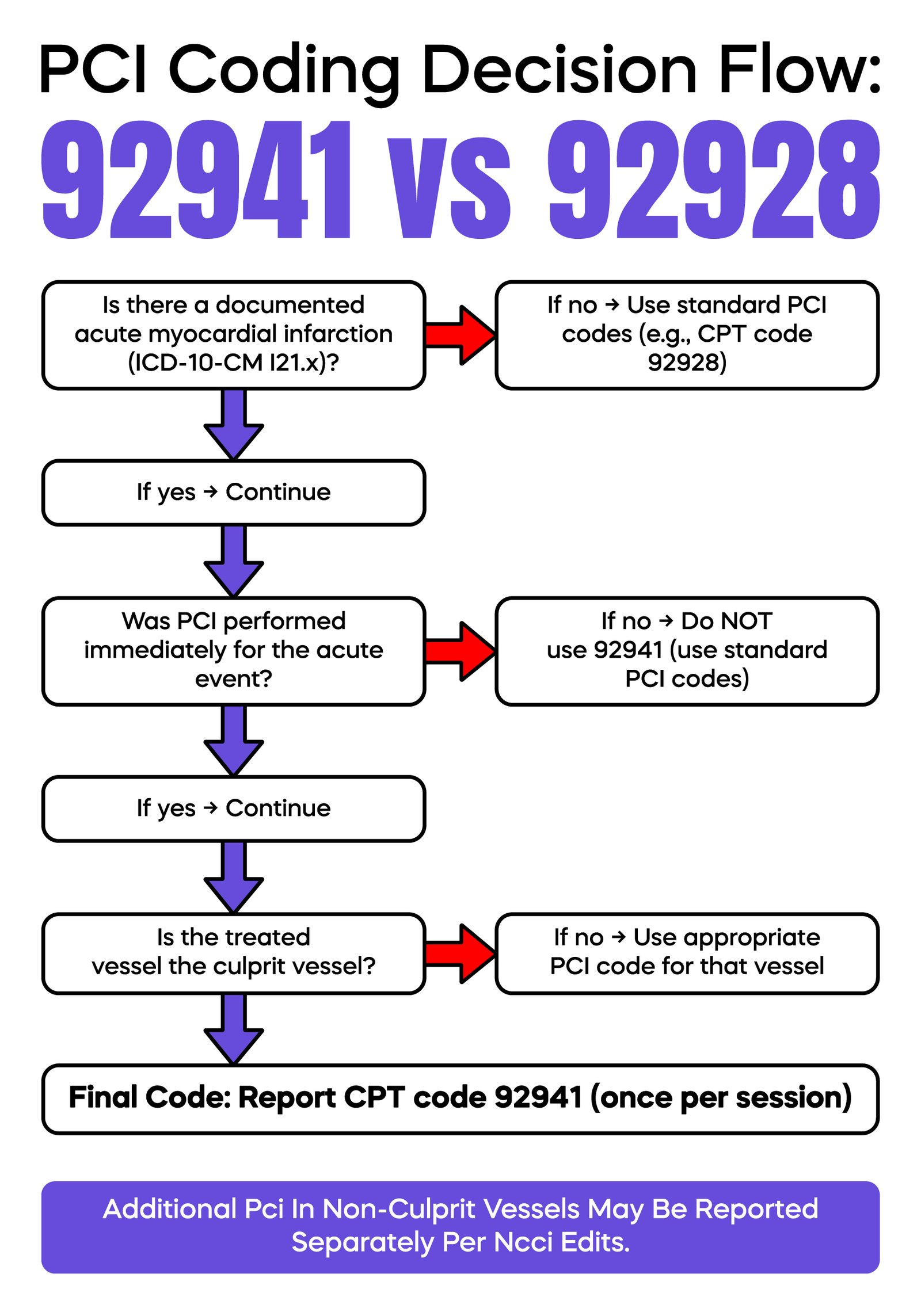
CPT code 92928 is used for PCI with stent placement in non-acute MI cases.
CPT code 92941 is used only when the PCI is performed during an acute myocardial infarction.
The difference is based on diagnosis, not just urgency.
A common denial occurs when 92941 is billed without linking it to an ICD-10-CM acute MI code from the I21.x category. In such cases, the payer often downcodes the claim to 92928.
Correct diagnosis linkage is essential for proper reimbursement.
| Criteria | CPT 92941 | CPT 92928 |
| Clinical Scenario | Acute myocardial infarction (STEMI/NSTEMI) | Stable or non-acute coronary disease |
| Diagnosis Requirement | Must link to I21.x (acute MI) | No acute MI required |
| Timing | Immediate intervention required | Can be elective, urgent, or staged |
| Vessel Rule | One culprit vessel only | Per vessel treated |
| Procedures Included | Angioplasty, stent, atherectomy | Stent placement |
| Documentation Risk | High audit risk if MI is not proven | Moderate |
| Common Denial Cause | Missing acute MI documentation | Incorrect modifier or bundling |
Code selection is based on diagnosis, not just urgency.
CPT code 92941 is a bundled code.
It includes vessel access, angioplasty, stent placement, atherectomy when performed, and completion angiography of the treated vessel. Standard intra-procedural medications are also included.
These services cannot be billed separately.
However, diagnostic coronary angiography may be separately billable, but only if it meets strict CPT criteria. This means it must represent a true diagnostic study. It should involve new clinical decision-making and should not be a repeat of prior imaging.
If the angiography is only part of the intervention, it is bundled and not separately payable.
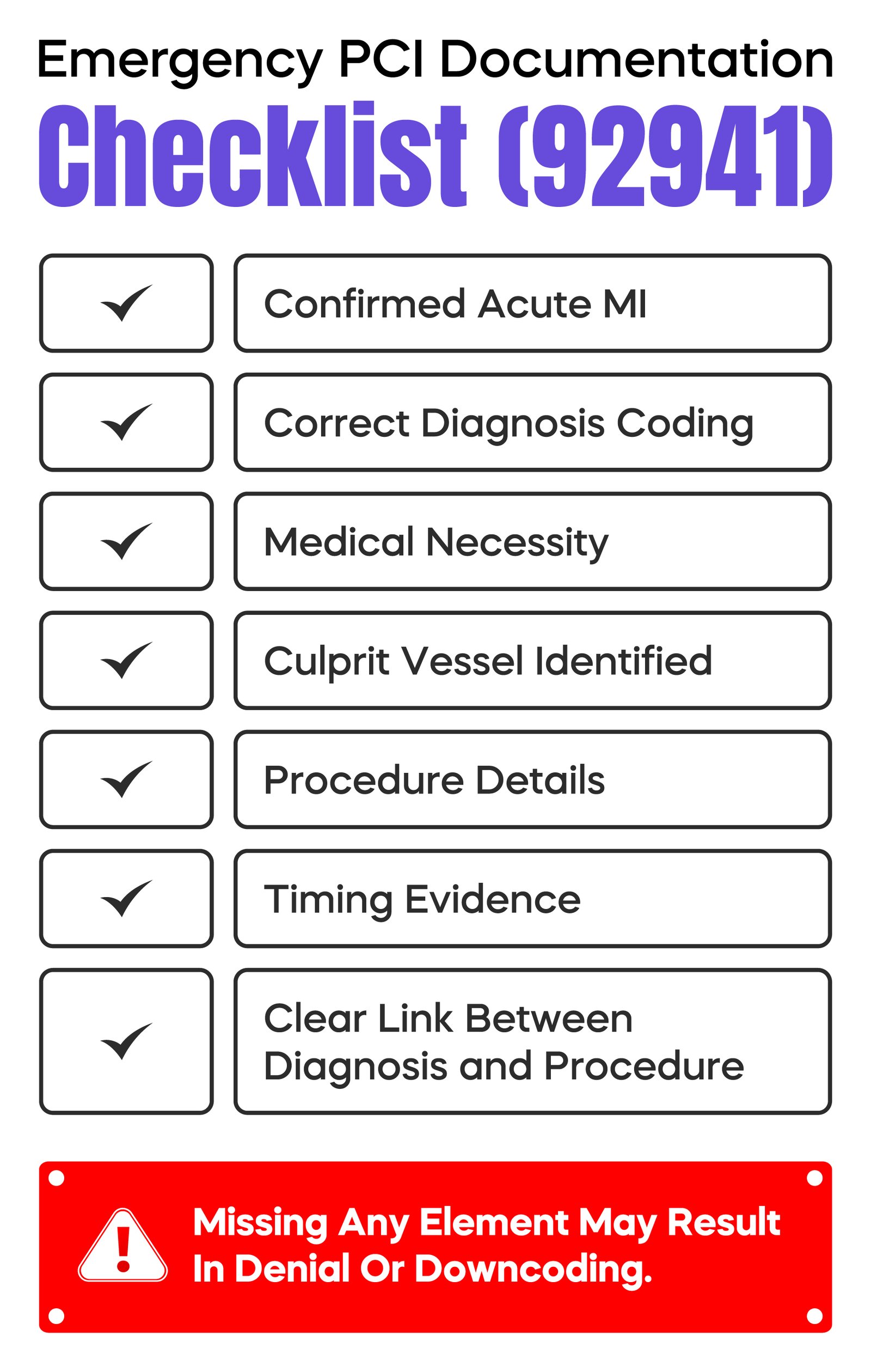
Strong documentation is essential for payment and audit defense.
Your note must clearly show an acute myocardial infarction. This should include symptoms, ECG findings such as ST elevation, and lab evidence like elevated troponin levels.
You must link the procedure to the correct ICD-10-CM acute MI codes, typically from the I21.x category.
The documentation should also describe the urgency and why immediate intervention was required.
Clearly identify the culprit vessel and describe the treatment performed.
Including timing details such as door-to-balloon time strengthens the case for medical necessity.
Without these elements, even a correct procedure may not be reimbursed.

Billing begins with complete and accurate documentation in the EHR.
The diagnosis must reflect an acute myocardial infarction using the appropriate ICD-10-CM code.
The claim is then prepared and submitted through the CMS-1500 form or electronic equivalent.
Clearinghouses often flag mismatches between diagnosis and procedure before submission.
Payers, especially Medicare contractors, review these claims carefully. They focus on medical necessity and documentation clarity.
If all elements align, the claim is paid. If not, it is denied or reduced.
Medicare reimburses CPT code 92941 when documentation supports an acute MI and immediate intervention.
Medicare Administrative Contractors apply local coverage policies and often review these claims closely.
Commercial payers follow similar logic but may apply additional edits.
Payment depends on documentation quality, diagnosis linkage, and compliance with coding rules.
Denials usually follow clear patterns.
One common issue is the missing documentation of acute MI. The fix is to clearly document clinical findings and link them to the procedure.
Another issue is incorrect code selection. Using 92941 without an acute MI leads to downcoding.
Improper code combinations also cause denials. While 92941 cannot be billed with 92928 for the same vessel, additional PCI codes may be reported for non-culprit vessels when appropriate and supported by documentation.
Modifier misuse is another trigger. Unsupported modifiers increase audit risk.
Each of these issues can be prevented with proper documentation and coding alignment.
Modifiers must be used carefully and based on documentation.
Anatomical modifiers such as LD, LC, and RC are often required by many payers, including several Medicare contractors, but this requirement is payer-specific. Practices should verify payer guidelines.
Modifiers such as 59 or XE may be used when a diagnostic angiogram is a distinct and separate service. This must be clearly supported in the record.
Incorrect modifier use is a common reason for audits.
Accurate billing starts during documentation.
Clearly state the diagnosis of acute myocardial infarction. Identify the culprit vessel and describe the intervention.
Ensure the clinical note supports the ICD-10-CM code used.
Communicate with your billing team when needed.
Regular internal reviews help identify patterns and prevent repeat errors.
CPT code 92941 is one of the most precise and high-risk codes in cardiology billing. It is not defined by how urgent the case feels, but by clear evidence of an acute myocardial infarction and immediate intervention on a single culprit vessel.
Most denials do not happen because the procedure was incorrect. They happen because the documentation does not clearly prove the emergency, the diagnosis is not properly linked using ICD-10-CM I21.x codes, or the code is used in situations that do not meet strict criteria.
To protect your revenue, focus on three things. First, document the acute MI clearly with clinical evidence. Second, identify and treat the culprit vessel with precise operative details. Third, align your coding with payer rules, especially when reporting additional vessels or using modifiers.
When these elements are in place, CPT code 92941 becomes straightforward to defend, even under audit. Without them, it becomes one of the fastest paths to denial and revenue loss in cardiology practice.
Arj Fatima is a senior medical billing and coding specialist with deep experience in U.S. cardiology billing and revenue cycle management. She works with physicians to reduce denials, improve documentation, and ensure compliance with Medicare and payer-specific rules. Her expertise includes PCI coding, audit defense, and real-world billing optimization.
© Billing MedTech. All Rights Reserved