Are you ready to grow up your business? Contact Us
Call us anytime
Are you ready to grow up your business? Contact Us
Doctors are tired of getting paid late for work that was done correctly. Claims are denied for small issues. Payments are reduced without a clear explanation. Staff spend hours fixing mistakes that could have been prevented. At the same time, audit pressure continues to grow.
Most denials are not clinical. They are administrative. A missing modifier. An outdated ICD-10-CM code. A documentation gap that fails to meet a Local Coverage Determination requirement. These errors start inside the practice, long before the claim reaches the payer.
AI Claim Scrubbing helps reduce these preventable denials. It reviews each claim before submission and estimates denial risk based on historical payer behavior and coding patterns. When implemented properly, practices often see preventable denials fall by up to 90 percent, and first-pass acceptance rates exceed 95 percent.
Insurance companies use advanced analytics to review claims. Federal programs under the Centers for Medicare and Medicaid Services and commercial payers rely on automated systems to scan every field of the CMS-1500 form.
These systems compare CPT procedure codes with ICD-10-CM diagnosis codes. They validate frequency limits. They review medical necessity rules under Local Coverage Determinations issued by Medicare Administrative Contractors.
If any inconsistency appears, the claim may be rejected, denied, or downcoded.
Many practices still depend on static rule-based scrubbing software. These programs follow fixed “if-then” logic. They do not adapt when payer behavior shifts. As payer analytics evolve, static tools fall behind.
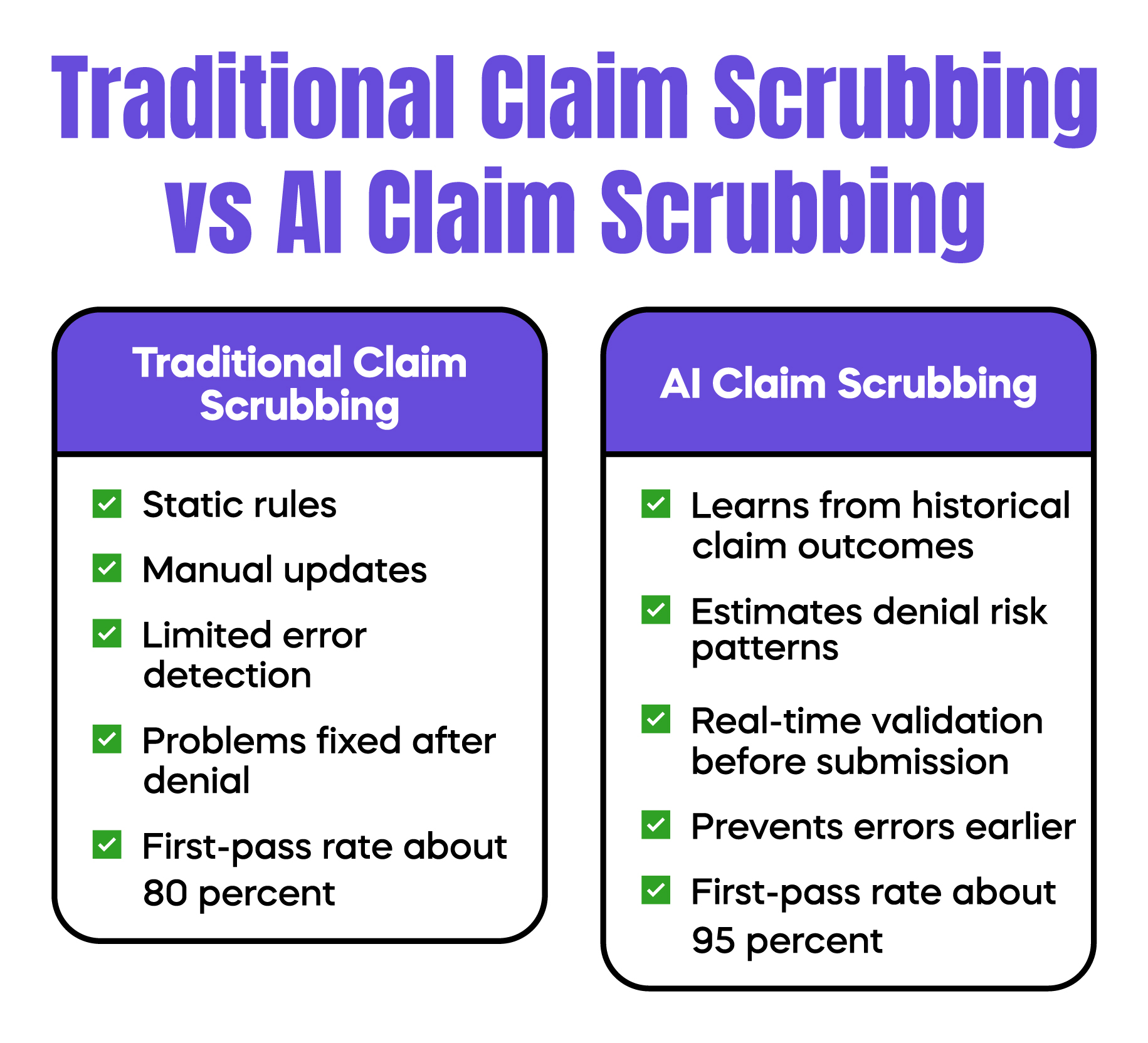
AI Claim Scrubbing uses machine learning models to analyze past claim outcomes. Instead of applying only fixed rules, it evaluates patterns in historical payer responses. It estimates denial risk based on combinations of CPT codes, ICD-10-CM codes, modifiers, provider type, and payer trends.
For example, if a payer recently increased denials for a specific modifier combination in a certain specialty, the system identifies that pattern. It alerts staff before submission.
The goal is not to guarantee approval. The goal is to reduce preventable risk before the claim leaves the practice.
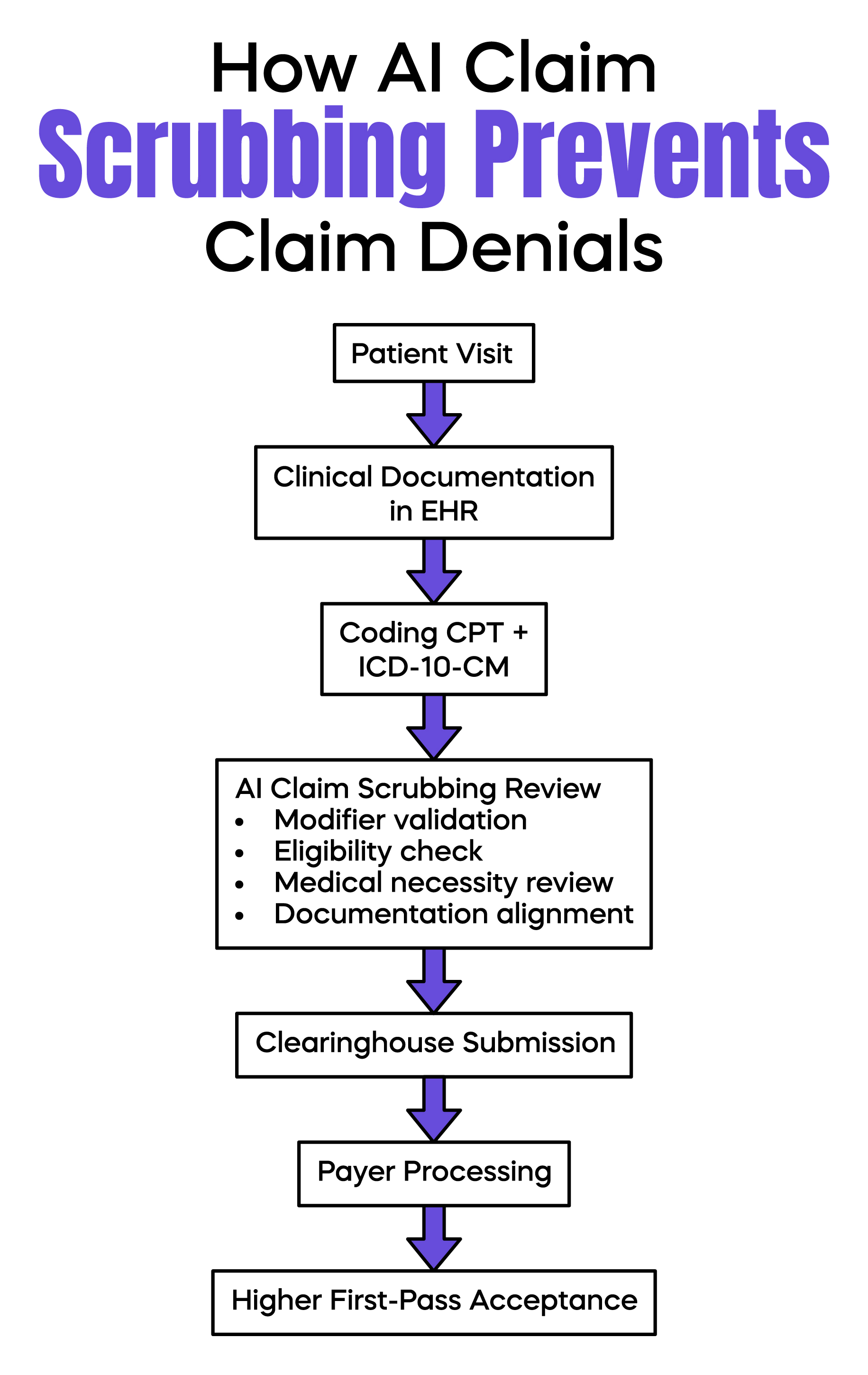
First-pass acceptance rate measures how many claims are processed without rework. In many practices, this rate stays between 75 and 85 percent. That means 15 to 25 percent of claims require correction.
AI Claim Scrubbing reduces this rework by validating several data layers at once. It checks patient demographics for accuracy. It verifies insurance eligibility data. It confirms that National Provider Identifier information matches enrollment records. It reviews prior authorization requirements when applicable.
When these checks occur before submission through the clearinghouse, rejection rates decrease. Fewer denials mean fewer appeals. Accounts receivable days shorten. Cash flow becomes more predictable.
Modifier misuse is a leading cause of denials. Modifier 25 allows separate payment for an evaluation and management service performed on the same day as a procedure. Modifier 59 indicates distinct procedural services. Both are closely monitored by payers.
AI systems review documentation complexity and compare it to the level of service billed. If documentation does not clearly support a separate evaluation, the system flags the claim for review.
For example, an orthopedic surgeon may perform a joint injection and also bill an office visit. If the visit documentation does not demonstrate a separately identifiable service, the claim carries risk. AI highlights this exposure before submission.
This reduces the chance of denial and lowers audit vulnerability.
Medical necessity denials often stem from weak diagnosis coding. ICD-10-CM requires detailed specificity, including laterality, severity, and encounter type.
AI Claim Scrubbing analyzes whether the diagnosis code logically supports the procedure billed. It references payer medical necessity policies and historical denial trends. If a diagnosis appears too vague or inconsistent with the service, the system estimates elevated denial risk.
This does not replace clinical judgment. It supports coding accuracy and documentation alignment.
Not all revenue loss appears as a denial. Sometimes a payer downcodes a service instead of rejecting it. A level 4 evaluation and management visit may be paid at a level 3 rate.
Advanced AI systems perform payment variance analysis. They compare expected contracted reimbursement with actual payment amounts. When patterns of downcoding emerge, the system flags them.
This allows the practice to identify systematic underpayment trends and address them through appeals or contract review.
Each denied claim requires staff time to research and correct. Industry estimates place the administrative cost of a single denial at approximately 25 dollars in labor.
For high-volume practices, these costs accumulate quickly.
AI reduces repetitive manual review by automating eligibility checks, coverage validation, and coding cross-analysis. Billing teams can focus on complex cases and compliance oversight rather than correcting preventable errors.
Revenue protection is important. Audit protection is critical.
Oversight bodies such as the Office of Inspector General use data analytics to identify billing outliers. Providers who consistently bill higher-level services compared to peers may attract scrutiny.
AI Claim Scrubbing can generate internal risk indicators. If a claim appears statistically unusual for a specialty, it is flagged for review. This internal screening process functions as a pre-submission compliance check.
By identifying potential outliers early, practices reduce exposure to post-payment audits and recoupments.
AI is a support tool. It is not a substitute for certified coding expertise.
Machine learning systems rely on accurate input data. If documentation is incomplete or inconsistent, predictions may be unreliable. Overdependence without review can create systematic errors.
The most effective approach is hybrid. AI handles high-volume validation and pattern analysis. Experienced coders perform final review on complex or high-value claims. This balance protects both revenue and compliance integrity.
AI tools must be configured according to the specialty. Cardiology billing patterns differ from dermatology or family medicine. Edits must align with clinical workflow.
Practices should monitor key metrics monthly, including clean claim rate, denial rate by payer, days in accounts receivable, and payment variance trends.
Staff education is essential. If alerts are ignored or routinely overridden, denial reduction will not occur. Clear policies should define when coder review is required.
First, AI often reveals undercoding patterns. Some physicians select lower-level codes out of caution. Data analysis may show that documentation supports higher compliant coding levels, increasing revenue without increasing patient volume.
Second, AI produces payer-specific performance intelligence. Instead of treating all insurers equally, the practice gains insight into which payer generates the highest denial or underpayment rate.
Third, structured denial risk data strengthens payer negotiations. Objective performance metrics improve leverage during contract discussions.
AI Claim Scrubbing does not promise guaranteed payment. It reduces preventable risk. It estimates denial probability based on historical payer behavior, coding combinations, and documentation alignment.
As payer analytics become more advanced, static billing workflows are no longer sufficient. Practices that combine intelligent automation with certified human oversight create a more stable revenue cycle.
For physicians facing rising denial rates and increasing audit pressure, AI-supported claim validation is becoming a structural safeguard rather than an optional upgrade.
Arj Fatima is a U.S. medical billing and revenue cycle management specialist with hands-on experience in denial prevention, coding audits, Medicare compliance, and payer contract analysis. She works closely with physicians, billing managers, and coders to reduce claim denials, strengthen documentation integrity, and protect practices from audit exposure. Her expertise focuses on practical systems that improve clean claim rates while maintaining strict regulatory compliance.
© Billing MedTech. All Rights Reserved